What is photodynamic therapy?
Cedars consultants are now the main providers of photodynamic therapy (PDT) for skin cancer in the private sector. We have completed original research showing the benefits of combining PDT with Mohs for optimal results in skin cancer.
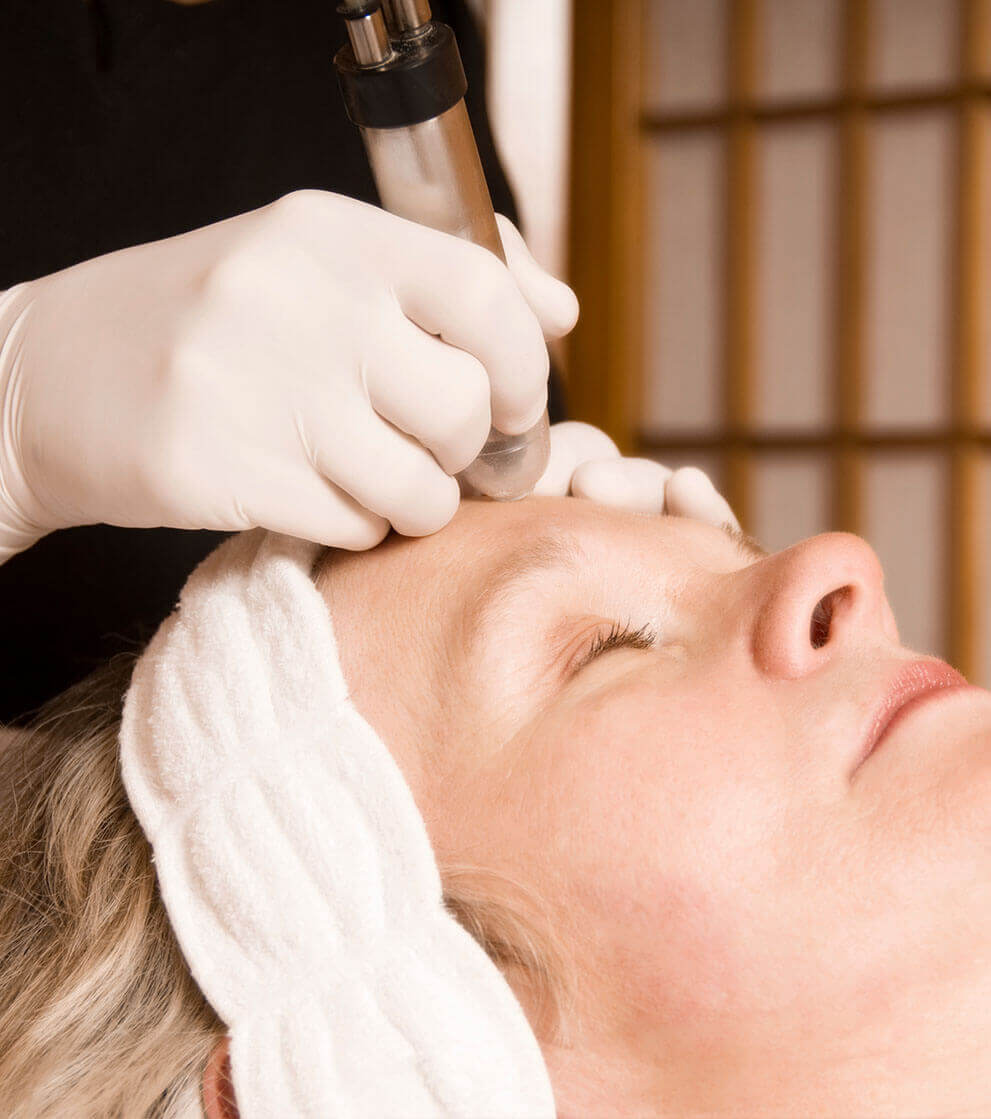
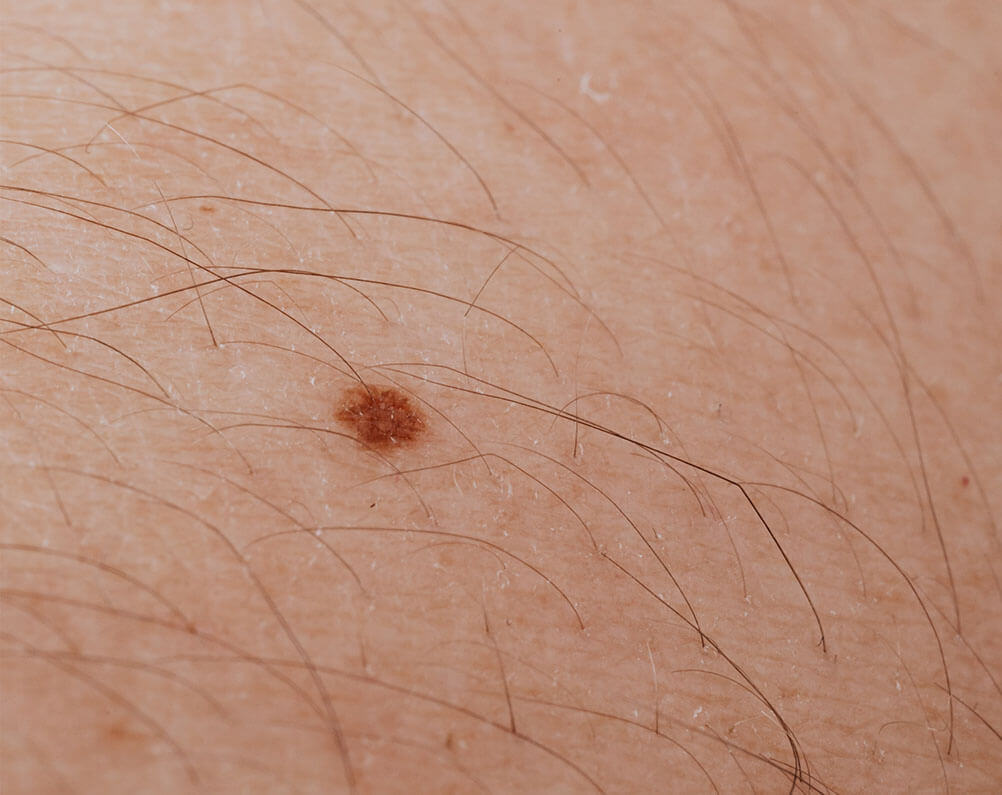
Photodynamic therapy (PDT) is a technique for treating skin cancers and sun-damaged skin which might one day turn cancerous (pre-cancers). In PDT a special light activates a cream which has been applied to the lesion (affected area of skin). This treatment kills the abnormal cells in the skin.
Book ConsultationWhat skin conditions can be treated with photodynamic therapy?
PDT can be used to treat various skin conditions including:
- Thin basal cell carcinomas
- Bowen’s disease (in situ squamous cell carcinoma), a pre-cancer.
- Actinic (solar) keratoses – early sun-damage, a pre-cancer

Your Consultation
At the Cedars Dermatology Clinic in Northwood & Harley Street, we draw deeply from the consultation process. Our expert clinicians will listen carefully to understand your skin concerns and aesthetic and medical goals.
- Your medical history is taken into account
- We thoroughly assess your skin
- We listen well to understand your concerns and goals
- We draw up a personalised treatment plan
FAQS about Photodynamic Therapy (PDT)
PDT involves the use of a light-sensitive chemical (called a photosensitiser). This photosensitiser is, by itself, harmless. When light of a certain wavelength (usually red light) is shone onto skin to which the photosensitiser has been applied, the photosensitiser is activated. This causes changes in the oxygen molecules within the sun-damaged skin cells. These “excited” oxygen molecules kill the cells. Only the area of skin exposed to the light source will be affected and inflamed; after the inflammation clears it should be cured.
PDT is an outpatient procedure, and will be done by your doctor or nurse. It takes several hours to complete. The first step is to apply a cream containing the photosensitiser to the area that needs to be treated. If necessary, any loose scale or crusts will be removed first. A dressing will then be applied over the cream and you will be asked to return in about 3 hours. This wait is to allow the photosensitiser to be absorbed and to be converted into the active chemical by the skin. The cream is then wiped off and the area cleaned. A bright coloured light is then shone onto the treatment area for approximately 10 to 45 minutes (the precise time will be determined by your doctor or nurse depending on the light source). After the treatment has been completed, a dressing will be applied for a minimum of 2 days, to prevent any further exposure to light.
Your doctor or nurse will explain how you should care for the treated areas. It is usually suggested that, after the dressing has been removed, you can wash, bathe or shower as usual. Do not rub the treated area, but gently pat it dry. Within a few days, a scab will form, and healing will take several weeks (depending on which part of the body has been treated).
Care must be taken not to scratch the area or accidentally dislodge the scab during the healing process. The use of a suitable sunscreen (SPF 30) following the procedure, especially during outdoor activities, is essential.
PDT is not recommended if you are pregnant.
The PDT cream may contain peanut oil, so tell your doctor and nurse if you are allergic to peanuts.
PDT is not recommended if you have porphyria (a light-sensitive disorder, where the patient is producing the same photosensitiser used in PDT and is present in the blood, skin and other tissues of the body).
Care should be taken not to get the dressing wet when bathing or showering.It is advisable to avoid swimming until the treated area is fully healed.
The short-term side effects of phototherapy include:
Pain. When the red light is shone onto the skin, the treated area may hurt. If it is too uncomfortable, your doctor or nurse may suggest pausing treatment for a while, or a local anaesthetic injection may be recommended. After completion of treatment, discomfort and itching may last for a few days, and may require pain-killers.
Inflammation. The treated area may initially become pink and puffy, and may ooze a little: this is a normal reaction. It settles within a few days.
Blistering and ulceration. The treated area may occasionally blister or ulcerate.
Infection. If the treated area becomes red, swollen and painful, an infection may have developed, and you should contact your doctor.
Potential long-term side effects of phototherapy include:
Scarring. There may be some scarring after PDT.
Colour change. The skin may be left darker or paler after PDT.
Treatment may not be effective, or the condition may come back again. If this happens, you may be offered further PDT, or an alternative type of treatment may be recommended.
Protect your skin with clothing, and don’t forget to wear a hat that protects your face, neck and ears, and a pair of UV protective sunglasses.
Spend time in the shade between 10am and 3pm when it’s sunny. Step out of the sun before your skin has a chance to redden or burn. Keep babies and young children out of direct sunlight.
When choosing a sunscreen look for a high protection’ SPF (SPF 30 or more) to protect against UVB, and the UVA circle logo and/or 4 or 5 UVA stars to protect against UVA. Apply plenty of sunscreen 15 to 30 minutes before going out in the sun, and reapply every two hours and straight after swimming and towel-drying.
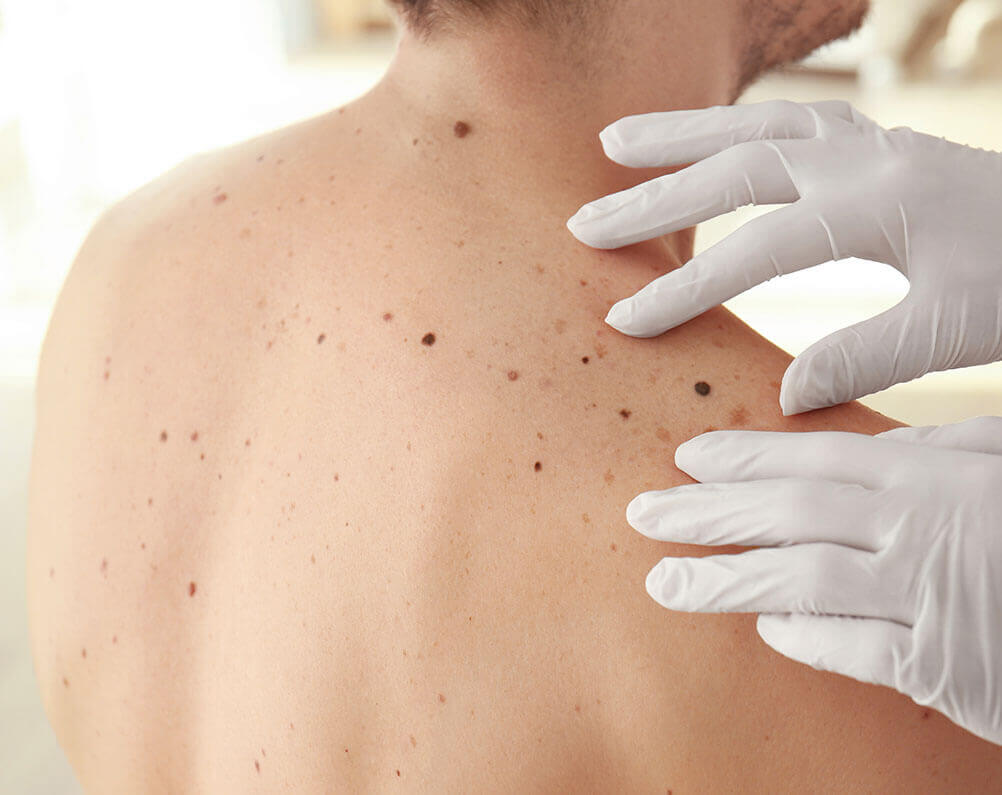
The British Association of Dermatologists recommends that you tell your doctor about any changes to a mole or patch of skin. If your GP is concerned about your skin, make sure you see a Consultant Dermatologist – an expert in diagnosing skin cancer.
Other treatments